- What is an otoplasty?
- Who is a candidate?
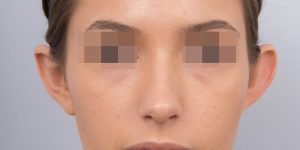
- Ear Surgery Photos
- What can you expect after the operation?
- What are the potential risks?
- Pre-operative Instructions
- Post-operative Instructions
What is an otoplasty?
An otoplasty is an operation to change the prominence or shape of the ears. Most commonly, the ears may stick out too far from the side of the head and is sometimes a family trait. Sometimes, the fold of the ear is underdeveloped or has completely failed to develop. In this instance, the operation involves taking a small amount of skin from behind the ear and then making cuts in the cartilage to weaken it and create a new fold. The other reason for surgery is when the ear has a very large conchal bowl (the cup-shaped area near the ear opening). Sometimes the operation involves reduction of this.
Our plastic surgeon—Dr Craig Layt—typically performs the operation as a day case. In children it is best performed under general anaesthetic. In adults it can be performed under a general anaesthesia however if specifically requested it can be performed under local anaesthesia with sedation. The operation attracts an item number from Medicare for under 18 and therefore some of the costs will be borne by Medicare and your Private Health Fund. All procedures, medical or cosmetic require a GP referral.
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified practitioner.
Who is a candidate?
People who have ears that stick out from the side of the head or whose ears have had an injury or genetics which may cause an undesirable shape are candidates for otoplasty. Children need to be old enough to understand the need to keep their bandages in place. A child older than 4-5 years of age is generally suitable depending on their maturity.
The aim is to surgically shape and position ears to a symmetrical shape and position and to also provide an anatomically balanced degree of fold, shape and protrusion from the side of the head.
Ear Surgery Photos
These before and after photos are of patients that have had surgery performed by Dr Layt. These patients have consented to the photos being shown. These are actual photos and have not been altered or digitally enhanced. Every patient is an individual and therefore final surgical results will vary from patient to patient.
What can you expect after the operation?
The ears will be bandaged in a turban-like fashion, which must remain in place for 10 days. It is not a particularly painful operation. Discomfort is usually controlled with oral medications. Children will occasionally vomit the evening after the procedure. This is a response to having their ears operated on. Generally, after 2 to 3 days there is very little discomfort.
An appointment will be made for the bandages to be removed at about a week to 10 days and you may then wash your hair. The ears will be a little swollen, red and bruised but this will settle rapidly. It is best to wear a headband at night for one month whilst healing continues to avoid bending the ears forward at night and affecting the final result. Contact sports should be avoided during this time.
What are the potential risks and complications?
Surgery is not an exact science. Incisions and scars are part of any surgery and the location and extent of the incisions will be discussed with you. Every effort is made by the surgeon to minimise scarring. Scars will fade over time, but they are permanent. They can also become hypertrophic or keloid. Scars vary from person to person and are related to each individual’s skin type, genetics and the ability of their skin to heal.
Every surgical procedure involves certain risks and complications (as per the ASPS brochure) including, but not limited to:
Asymmetry is evident physically in every person. No two sides of the body are ever exactly symmetrical in shape, position or size and the surgeon will make every effort to achieve as close to symmetry as possible but some asymmetry is normal.
Delayed Healing, Infection and Suture Reactions can all be possible healing issues and may require antibiotics or in some cases surgical exploration.
Bleeding, Haematoma or Seroma Collections may resolve themselves but, in some cases may require further surgery.
Loss of Sensation and Numbness may also be experienced. In most cases this will improve over time on its own. In some cases this can be permanent.
Bruising and Swelling may also be a short term effect from surgery and will usually settle in one to two weeks.
Allergies to dressings, medical lotions, sutures or other materials can occur with some patients. You will be advised to cease the use of the dressing, lotion or material that is causing the reaction. In some cases anti-inflammatory medication may be prescribed.
Breathing Difficulties may be due to a general anaesthetic or breathing tube during the operation which has caused some swelling, noisy breathing or discomfort.
Blood Clots can also occur in some surgeries and may require urgent treatment and hospitalisation.
Pain thresholds vary from patient to patient. This may lead to different pain management and/or different recovery times to resume normal activities.
Achieving realistic results with minimal risk is a joint effort. It is important to disclose all information to the surgeon and clinic and to understand the following:
Full disclosure of your medical history including: allergies, personal, physical and mental history, previous surgeries, current medications and co-morbidities (including but not limited to, smoking, vaping, diabetes, prescription and illegal drug addictions, blood or heart disease, obesity or anorexia).
Co-morbidities may impact on outcome and healing post surgery.
Smoking, vaping, or taking recreational drugs must be ceased in the 6 weeks prior to some operations and during the healing phase. Failure to do so may increase the risk of complications, decrease your healing ability and affect your surgical outcome.
You should not take aspirin based prescription drugs 14 days prior to surgery and during the healing phase of the operation unless advised otherwise by the surgeon.
As per the Australian Health Practitioner Regulation Agency (AHPRA), all non-rebatable (cosmetic) procedures require a validated screening of Body Dysmorphia to be undertaken.
If Dr Layt is concerned about your mental state or physical state prior to the procedure, he may request evaluation by a psychologist, psychiatrist, general practitioner or other specialist. This referral is to assess your suitability, increased risks during surgery or any underlying physical or psychological problems which may affect your recovery or mental health.
In some cases this may require surgery to be postponed or cancelled by the doctor in his primary role to consider your care and personal well-being.
All surgery carries risks and it is important to understand these.
Every patient is an individual and therefore final surgical results will vary from patient to patient. Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified practitioner.
Specific Pre-Operative Instructions
WASHING: Wash the evening prior to surgery and the day of surgery paying particular attention to the ear region and hair. The area behind the ears should be carefully washed. This decreases the bacterial count and should decrease the risks of infection.
PRODUCTS: Do not apply moisturisers, make-up, perfume/deodorant, nail polish or hair products after washing. Remove all jewellery.
CLOTHING: Wear loose, comfortable clothing and footwear. A shirt with a button or zipper opening is ideal for removal.
HEADBAND: You will be required to wear a headband for 4-6 weeks post-operatively while you sleep. This will be supplied in your post operative pack.
HAIR: If you have long hair it should be tied up in a pony tail on top of the head using a simple elastic band. This will keep it out of the way during surgery and make dressings easier to apply.
FASTING: You should have nothing to eat or drink for 6 hours before your operation. If you are required to take medication during this time please speak with your physician to check if this can be taken before the 6 hour fasting period or after your procedure.
SMOKING: Smoking and vaping increases the risks of complications significantly and should be ceased 6-8 weeks prior to surgery.
MEDICATION: If you are having the operation as a day case, you will be given a script for antibiotics and pain relief tablets that you will need to purchase from the chemist and bring with you on the day of your procedure. Do not take these prior to surgery. The nursing staff will advise you and your carer after your procedure on how to administer them.
Certain over the counter products and prescription medicines can cause complications before and after surgery. They can reduce the ability of your blood to clot and could increase your tendency to bleed during and after surgery. Do not take any medication containing or related to aspirin 2 weeks prior to your procedure. This includes NSAID’S, anti-Inflammatory medications, blood thinning medication. Please see your doctor regarding if and when to cease medication. *This is not an all inclusive list*.
Also avoid Vitamin E supplements and red wine. Stop all herbal medications before surgery. The most common herbs used are Echinacea, Ephedra, Garlic, Ginseng, Ginkogo, Kava, St. John’s Wort, and Valerian. They may adversely effect anesthetic drugs, prolong bleeding and impair healing after surgery. Please consult your physician before ceasing any medication.
ADMINISTRATION: Unfortunately, paperwork is a necessary evil. Each theatre complex has its own procedures. We have attempted to make it all easy by providing a simple series of steps to follow titled “THINGS TO DO FOR YOUR PROCEDURE” specific to the surgery centre you are attending. Please follow these instructions. If you have any queries about this or anything else don’t hesitate to contact us on 55974100.
Specific Post-Operative Instructions
POSITION: Elevate your head to decrease the swelling. Try to sleep on your back if possible.
DRESSINGS: Do not remove the dressings. If they appear to be falling off or become loose contact our clinic. Once the dressings are removed on day 7 – 10, avoid pulling on the stitches or bending the ear forward.
HEADBAND: Wear the headband over the ears when sleeping for 4 – 6 weeks after surgery. This will be supplied in your post-operative pack.
TED STOCKINGS: You may be required to wear TED stockings for compression to prevent DVT (blood clotting) post-operatively. If required these will be fitted at the hospital on your admission day. The nursing staff will advise you on how long you need to wear these for.
MEDICATION: Take your pain relief and antibiotic medication as directed. Any medication you ceased prior to surgery must not be taken after your surgery until you are completely healed or as directed by your physician.
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.