It is very common for women to experience a loss of firmness and projection in the breasts over time. A breast lift procedure can directly address signs of breast ptosis (sagginess) to reposition the breasts. Breast lift surgery is one of the most popular procedures performed by our plastic surgeon here at The Layt Clinic. With a customised breast lift treatment from Dr Craig Layt, you can reposition and lift your breasts.
- What is a Breast Lift?
- Breast Lift Benefits
- Breast Lift Before-and-After Photos
- Breast Lift Candidates
- Breast Lift Procedure
- Breast Lift Recovery
- Breast Lift Scars
- Breast Lift Results
- Breast Lift Risks
- Breast Lift Cost
- Additional Breast Lift FAQs
- Breast Lift Pre-Operative Instructions
- Breast Lift Post-Operative Instructions
Meet Our Surgeons
Dr Craig Layt
Specialist Plastic Surgeon
- ASPS
- RACS
- NZMC
- FRACS
- AMC
Dr Layt is highly credentialed in many areas of Plastic, Cosmetic, and Reconstructive Surgery, as well as a variety of non-surgical cosmetic enhancements.
Dr Paul Ting-Yuan Cheng
Specialist Plastic Surgeon
- FRACS
- MBChB
- BHB
- PGDipSurgAnat
- ASAPS
- RACS
- NZAPS
Dr Cheng is a New Zealand trained Specialist Plastic, Aesthetic and Reconstructive Surgeon. He enjoys various aspects of plastic & reconstructive surgery, including aesthetic facial surgery / breast & body contouring surgery / burn & trauma reconstruction / microsurgery / hand surgery, etc.
What is a Breast Lift?
A breast lift (mastopexy) procedure is designed to correct the issues associated with the inferior descent of the nipple in relation to the breast fold and the lower redundant breast tissue – which is technically referred to as “breast ptosis.” The development of excess, inelastic breast skin can eventually cause the breasts to descend, leading to a ptotic appearance. This may be due to genetics, the natural ageing process, weight loss, pregnancy, and/or environmental factors. In minor degrees of ptosis, the sagging may be addressed by the insertion of breast implants; however, if the degree of breast ptosis is significant, breast lift surgery may be performed to address the position of the nipples and breast tissue and bring them to a higher projection. A breast lift can be performed on its own, or a breast lift with implants procedure may be recommended in cases where additional volume is also desired. Occasionally, fat grafting may also be advised in order to further address breast shape and symmetry. If you feel your breasts are too large, Dr Layt may suggest a breast reduction, which is also capable of providing a degree of “lift” to the breasts. Dr Layt will talk with you about your concerns and help you determine the best option for your unique needs.
What are the Benefits of Breast Lift Surgery?
Breast lift surgery can modify the appearance of the breasts by:
- Reducing excess, inelastic skin and tightening the remaining skin
- Lifting the breasts and nipples to a higher location, which can present more breast projection
- Recontouring and reshaping the breasts
- Centralising the location of the nipples
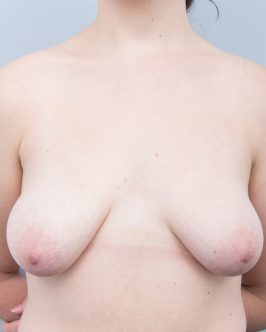
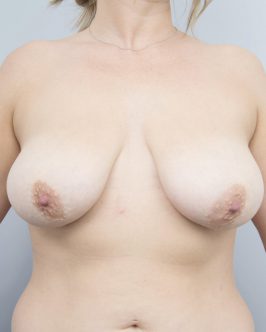
Breast Lift Before-and-After Photos
These before-and-after photos depict the results of breast lift surgery performed by Dr Layt. These patients have consented to the photos being shown. The images are actual photos and have not been altered or digitally enhanced. While every individual is unique and the final surgical results will vary from patient to patient, these photos can provide a general idea as to the outcomes that have been experienced with this treatment.
Am I a Candidate for Breast Lift Surgery?
Suitable candidates for breast lift surgery typically include women who are experiencing breast ptosis due to pregnancy, ageing, weight loss, genetics, or other factors. Dr Layt will consult with you to assess if this surgery is the right option for your needs. Women who would like to address large areolae may also be good candidates for this procedure since it can be an effective option for reducing areolae size.
During your consultation with Dr Layt, the breasts will be examined for the degree of breast ptosis that is present. It is important to determine the precise level of descending breast tissue because this will indicate which breast lift technique can be the most ideal for your specific needs.
Degrees of Breast Ptosis
Pseudoptosis (Glandular Ptosis)
Pseudoptosis, sometimes referred to as “glandular ptosis,” is the mildest form of breast ptosis. It is characterised by breasts that are falling just below the inframammary fold (the crease where the lower area of the breast meets the chest), but the nipples are still above the fold.
Grade I Ptosis
This degree of breast ptosis is slightly more severe than pseudoptosis. Grade I ptosis is characterised by breasts that have descended below the inframammary fold and nipples that appear at the same level as the fold.
Grade II Ptosis
This grade of ptosis indicates breasts and nipples that have sagged below the inframammary fold.
Grade III Ptosis
The most severe degree of breast sagginess is known as Grade III ptosis. This level of ptosis is diagnosed when the breasts and the nipples are sagging significantly below the inframammary fold and the nipples are pointing downward.
Once Dr Layt has talked with you about your concerns and performed an evaluation, he can determine whether you are an ideal candidate for breast lift surgery and explain the techniques which may be most suitable for your needs. If you are interested in adding volume to your breasts in addition to a breast lift, he can talk with you about whether breast augmentation is also worthy of consideration.
What Does the Breast Lift Procedure Involve?
The breast lift procedure typically requires general anaesthesia; however, most patients can return home on the same day as the surgery. There are a number of breast lift techniques that can be utilised; Dr. Layt will determine the technique that will be necessary based on the level of breast ptosis you are experiencing and what is best for your unique needs and goals. In most cases, the breast lift will involve incisions that begin in the areolar regions and extend downward to the inframammary fold. Excess tissue will be removed and Dr Layt will then tighten the remaining skin. The breasts and nipples will be quite literally “lifted” to a higher position and carefully shaped and smoothed.
It is important to note that any surgical or invasive procedure carries risks. We will explain all of the potential risks, however rare they may be, during your initial consultation. Before proceeding, you should seek a second opinion from an appropriately qualified practitioner.
What Can I Expect During Breast Lift Recovery?
During recovery, you can expect a certain level of soreness, swelling, and bruising in the surgical areas. The breasts may have patchy areas of numbness during the early post-operative period. Tingling, burning, or shooting pains generally indicate healing and should not alarm. Some asymmetry is normal after the operation as each breast swells to a different degree. The breasts will often appear a little flat at the bottom for a period after surgery. This is normal and is done on purpose as the breasts tend to bottom out more with time. Pain experienced in the course of the healing process can be controlled by oral medications. Some individuals are able to resume work or other non-strenuous activities after approximately one week of rest at home; however, others may need at least two weeks before returning to their normal daily routines.
Drains are rarely used and not often required. Sutures are placed under the skin and are dissolvable. We will schedule a follow-up appointment 24 – 48 hours after the breast lift operation to review your dressings, medications, and exercises. You will also be seen approximately seven days post-surgery to change dressings and review your surgical progress. Light activities can be resumed as tolerated—our plastic surgery team will provide you with detailed instructions and recommendations. Aerobic activities can be started in approximately three weeks. We are always available to help should concerns arise. We also recommend that we see you for a three-month and 12-month follow-up appointment. If distance to our practice is a problem, we can often address these issues over Skype, FaceTime, or telephone.
How Noticeable are Breast Lift Scars?
Breast lift surgery will produce some degree of scarring; however, the extent and noticeability of breast lift scars will depend on the specific technique that is performed. For milder cases of breast ptosis, a technique such as a “donut” mastopexy may be ideal, which involves incisions around the areola. This typically results in a barely noticeable scar since it often blends in with the skin surrounding the nipple. However, many breast lift patients require a more traditional mastopexy technique, which involves incisions created around the areola down to the crease of the breast and along the breast fold. This technique will result in noticeable scars; however, Dr Layt has performed breast lift procedures many times and utilises suturing techniques designed to minimise their appearance as much as possible. Also, our practice offers a number of scar management options that can help reduce the visible signs of scarring. Additionally, it should be noted that residual scars should fade to a certain degree over time.
How Long Does a Breast Lift Last?
The results of a breast lift can last for many years as long as some general precautions are taken. Please keep in mind that the natural ageing process will continue to have an effect on the appearance of the breasts as time passes; however, these effects can be slowed and breast lift outcomes can be maintained for extended periods by limiting weight fluctuations, sticking to a healthy diet, wearing high-SPF sunscreens while out in the sun, refraining from smoking, and avoiding tanning booths. It is also recommended to wear a supportive bra as consistently as possible.
What are the Potential Risks of Breast Lift Surgery?
Risks and Complications
Surgery is not an exact science. Incisions and scars are part of any surgery and the location and extent of the incisions will be discussed with you. Every effort is made by the surgeon to minimise scarring. Scars may fade over time, but they are permanent. They can also become hypertrophic or keloid. Scars vary from person to person and are related to each individual’s skin type, genetics and the ability of their skin to heal.
Every surgical procedure involves certain risks and complications (as per the ASPS brochure) including, but not limited to:
Asymmetry is evident physically in every person. No two sides of the body are ever exactly symmetrical in shape, position or size and the surgeon will make every effort to achieve as close to symmetry as possible but some asymmetry is normal.
Delayed Healing, Infection and Suture Reactions can all be possible healing issues and may require antibiotics or in some cases surgical exploration.
Bleeding, Haematoma or Seroma Collections may resolve themselves but, in some cases may require further surgery.
Loss of Sensation and Numbness may also be experienced. In most cases this will improve over time on its own. In some cases this can be permanent.
Bruising and Swelling may also be a short term effect from surgery and will usually settle in one to two weeks.
Allergies to dressings, medical lotions, sutures or other materials can occur with some patients. You will be advised to cease the use of the dressing, lotion or material that is causing the reaction. In some cases anti-inflammatory medication may be prescribed.
Breathing Difficulties may be due to a general anaesthetic or breathing tube during the operation which has caused some swelling, noisy breathing or discomfort.
Blood Clots can also occur in some surgeries and may require urgent treatment and hospitalisation.
Pain thresholds vary from patient to patient. This may lead to different pain management and/or different recovery times to resume normal activities.
Achieving satisfactory results with minimal risk is a joint effort. It is important to disclosed to the surgeon and clinic and understand the following:
Full disclosure of your medical history including: allergies, personal, physical and mental history, previous surgeries, current medications and co-morbidities (including but not limited to, smoking, vaping, diabetes, prescription and illegal drug addictions, blood or heart disease, obesity or anorexia).
Co-morbidities may impact on outcome and healing post surgery.
Smoking, vaping, or taking recreational drugs must be ceased in the 6 weeks prior to some operations and during the healing phase. Failure to do so may increase the risk of complications, decrease your healing ability and affect your surgical outcome.
You should not take aspirin based prescription drugs 14 days prior to surgery and during the healing phase of the operation unless advised otherwise by the surgeon.
As per the Australian Health Practitioner Regulation Agency (AHPRA), all non-rebatable (cosmetic) procedures require a validated screening of Body Dysmorphia to be undertaken.
If Dr Layt is concerned about your mental state or physical state prior to the procedure, he may request evaluation by a psychologist, psychiatrist, general practitioner or other specialist. This referral is to assess your suitability, increased risks during surgery or any underlying physical or psychological problems which may affect your recovery or mental health.
In some cases this may require surgery to be postponed or cancelled by the doctor in his primary role to consider your care and personal well-being.
Complications with Breast Implants
Pregnancy may cause breast enlargement, cause the breast tissue to stretch, and a degree of ‘drooping’ of the breast tissue. This may require the breast to be surgically lifted; however, some poor skin integrity may have a tendency to stretch and continue to ‘drop’.
Capsular Contracture (less than 1%) occurs when the scar surrounding the implant thickens and tightens around the implant. This can make it feel hard, look unnatural, feel uncomfortable and may occur months to years later. Should this occur, a capsulectomy and a remove and replacement of implant(s) may be required in the future.
Implant Rupture can occur after injury or years of repetitive action in the same part of the implant. MRI is the gold standard to assess this as Ultrasound shows a false positive reporting for rupture in approximately 30% of cases. A ruptured or leaking implant will require surgery of removal and replacement of the implant.
Implant ‘Wrinkles’ and Palpability can also be noticed. All implants ripple to a degree. If there is reasonable tissue coverage this will not be noticeable. If there is little overlying breast tissue and fat this is more likely.
Anaplastic Large Cell Lymphoma (ALCL) is a rare tumour of lymphoid cells in the breast which has recently been found to have an increased incidence in patients with textured breast implants. ALCL relates to a patients genetics, a textured implant and bacteria being present. This may present as a unilateral swelling of a breast due to fluid accumulation. When detected early, this is treated by removing the fluid and the implant. Dr Layt has and continues to perform this procedure utilising the 14 point plan to minimise the risks of ALCL, capsular contracture and other complications relating to using an implant.
In summary, the risks of bleeding, haematomas, capsular contracture, ALCL, infection, asymmetry, scarring, seroma, pain, palpable implant, loss of cleavage, sensation, implant malposition, implant rupture/leakage and breast feeding are discussed through the ASPS and The Layt Clinic information on Breast Augmentation. Implants may be removed and replaced over time and they are not lifetime devices. Implants used are registered with the Therapeutic Goods of Australia (TGA) and patients will be sent Patient Information Leaflet (PIL) regarding the implants chosen.
All surgery carries risks and it is important to understand these.
Every patient is an individual and therefore final surgical results will vary from patient to patient. Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified practitioner.
Modern surgery has developed over the years and the safety of surgery has improved greatly. There is however no such thing as “risk-free” surgery. The important thing is to understand any potential risks and minimise their occurrence by appropriate planning and management. Some specific possible risks include a lack of nipple sensation and asymmetry of the breasts after healing. Obviously, there will be some scars, and we will discuss how to minimise signs of them. At your consultation, the risks and potential complications of breast lift surgery will be explained and you will be given detailed information on the procedure.
How Much Does a Breast Lift Cost?
The total cost of a breast lift (without the addition of implants) at our practice typically falls in the range of $13,500 to $18,500—this includes the surgeon’s fee, anaesthetic fee, and operating theatre fee. Please note that this estimation of fees is subject to change. A firm quote can only be provided after your initial consultation with the surgeon. The cost of breast lift surgery can vary significantly from one patient to another based upon the specifics of their customised treatment plan. Ultimately, a number of factors will be taken into account for the final cost, including the breast lift technique utilised, whether breast implants will be placed in addition to the breast lift, the overall complexity of the procedure, the surgeon’s fee, costs associated with anaesthesia and use of the operating theatre, and other components. The total estimated cost of your breast lift surgery will be calculated once your treatment plan is developed during the initial consultation so that you have a full understanding of the financial obligations before the procedure takes place. A member of our team will be happy to answer any questions you may have about the many convenient payment methods we accept at The Layt Clinic.
Breast Lift Pre-Operative Instructions
WASHING:
Wash the evening prior to surgery and the day of surgery, paying particular attention to the breast region. This decreases the bacterial count and should decrease the risks of infection.
PRODUCTS:
Do not apply moisturisers, make-up, perfume/deodorant, nail polish, or hair products after washing. Remove all jewelry.
CLOTHING:
Wear loose, comfortable clothing and footwear. A shirt with a button or zipper opening is ideal for removal.
SMOKING:
Smoking and vaping increases the risks of complications significantly and should be ceased 6 – 8 weeks prior to surgery.
FASTING:
You should have nothing to eat or drink for six hours before your operation. If you are required to take medication during this time, please mention this to us to check if this can be taken before the six-hour fasting period or after your procedure.
MEDICATION:
If you are having the operation as a day case, you will be given a script for antibiotics and pain relief tablets that you will need to purchase from the chemist and bring with you on the day of your procedure. Do not take these prior to surgery. The nursing staff will advise you and your carer after your procedure on how to administer them.
Certain over-the-counter products and prescription medicines can cause complications before and after surgery. They can reduce the ability of your blood to clot and could increase your tendency to bleed during and after surgery. Do not take any medication containing or related to aspirin two weeks prior to your procedure. This includes NSAIDS, anti-inflammatory medications, and blood thinning medications. Please see your doctor regarding if and when to cease this medication. Ibuprofen, Nurofen, and Aspirin are common medications that thin the blood. *This is not an all-inclusive list*.
Also avoid Vitamin E supplements and red wine. Stop all herbal medications before surgery. The most common herbs used are Echinacea, Ephedra, Garlic, Ginseng, Ginkogo, Kava, St. John’s Wort, and Valerian. They may adversely affect anaesthetic drugs, prolong bleeding, and impair healing after surgery. Please consult your physician before ceasing any medication.
ADMINISTRATION:
Unfortunately, paperwork is a necessary evil. Each theatre complex has its own procedures. We have attempted to make it all easy by providing a simple series of steps to follow titled “SURGERY CHECKLIST” specific to the surgery centre you are attending. Please follow these instructions. If you have any queries about this or anything else don’t hesitate to contact us on (07) 5597 4100.
Breast Lift Post-Operative Instructions
POSITION:
For the first week after surgery, try to sleep on your back if you can instead of your side. Obviously, try not to sleep on your new breasts. This will help reduce swelling. (It is more important for you to sleep than to rigidly adhere to this suggestion).
DRESSINGS & DRAINS:
Drains are rarely/if ever required. You may have ‘splash proof’ dressings over your suture sites. Your pain will be controlled by oral medications. You will have an appointment to see us 24 – 48 hours after the operation for review of dressings, medications, and exercises. You will also be seen approximately seven days post-surgery to change dressings and review your surgical progress. Light activities can be resumed as tolerated. Aerobic activities can be started in about three weeks. We are always available to help should concerns arise. We would love to see you for a three month and 12-month follow-up appointment. If distance is a problem, we can often address this over Skype, FaceTime, or phone.
You will be fitted with a support bra and when we see you post-operatively we will check that it fits well and supply a second one. You should wear one of these day and night for two weeks after surgery. (You may, of course, remove it to shower and launder.) After two weeks, you may sleep without the bra. You should not go braless during the day for 4 – 6 weeks after surgery. Once the swelling has decreased you can buy new bras to fit your new size. This usually takes three months.
SHOWERING:
You may shower, remembering that your dressings are splash proof rather than waterproof. If water gets underneath the dressing it is best to change it. It is fine to take off your bra while you shower.
DRIVING AND ACTIVITIES:
You may take a gentle walk the day after your surgery. It is advised to try to get up and move about as soon as you feel you can. Do not return to aerobic exercise for three weeks. You may drive when driving does not cause you pain, and your vision, reflexes, and thought processes are not impaired and you are confident in your driving ability. This usually occurs in 4 – 6 days if you have a car with power steering.
SUTURES:
The sutures used in the operation are usually dissolvable and don’t require removal.
SUNLIGHT: Scars take at least one year to fade. During this time, you must protect them from the sun. Even through a bathing suit, a good deal of sunlight can reach the skin and cause damage. Wear a sunscreen with a skin-protection factor (SPF) of at least 30 at all times when in the sun. Be extremely careful as areas of your breast skin may have reduced sensitivity.
TAPE:
Dr Layt advises taping the wounds with Fixomull® initially, then Siltape® for 8 – 12 weeks after your operation for optimal scar healing. Our nurse will change these dressings one week after your operation. You will be given a pack of Siltape that will usually last until your 3-month appointment. Further Siltape is available for purchase. If any redness, itchiness or heat is noticed around the edges of the tape or wound please contact our clinic. Some patients may require to use different taping or silicone gels due to allergies to particular adhesives in some tapes.
TED STOCKINGS:
You may be required to wear TED stockings for compression to prevent DVT (blood clotting) post-operatively. If required, these will be fitted at the hospital on your admission day. The nursing staff will advise you on how long you’ll need to wear these.
MEDICATION:
Take your pain relief and antibiotic medication as directed. Any medication you ceased prior to surgery must not be taken after your surgery until you are completely healed or as directed by your physician.
Additional Frequently Asked Questions About Breast Lift Surgery
Will insurance cover breast lift surgery?
Mastopexy is typically categorised as a cosmetic procedure and generally not covered by medical insurance policies. Medicare may cover some mastopexy procedures and have a strict criteria which must be met. Once the surgeon has clinically assessed you, we will know if you meet the criteria and if you are entitled to a Medicare rebate. However, there are many options that can provide individuals with convenient ways to bring this treatment into their budget. Please visit our financing page for more information.
Will I need breast augmentation with my breast lift?
If a patient desires larger shaped breasts in addition to addressing concerns relating to breast ptosis, it’s quite common to perform an augmentation mastopexy. However, a mastopexy with breast augmentation is much more complex, so this procedure should always be under the care of a qualified and credentialed plastic surgeon, such as Dr Layt. During the initial consultation, Dr Layt will discuss the patient’s aesthetic goals and perform a breast examination to determine if augmentation mastopexy is a favourable option.
How painful is a breast lift?
Mastopexy procedures are performed under general anaesthesia, so the patient should be unaware of any discomfort during surgery. Most patients do experience some degree of soreness, swelling, and tenderness in the breast areas near the incisions in the days, or possibly weeks, following the procedure. These symptoms should subside gradually during the recovery process and can typically be well-managed with oral pain medication as needed.
How can I reduce swelling after a breast lift?
Swelling is the body’s natural response to incisional surgery, so this side effect is to be expected. There are a few ways to help minimise swelling, including wearing a compression garment, restricting salt and alcohol intake, eating a healthy diet of antioxidant-rich and anti-inflammatory foods, staying hydrated, getting plenty of rest, and taking light walks under the guidance of post-procedure clearance.
What type of bra should I wear after breast lift surgery?
A surgical support bra or compression garment should be worn immediately following the breast lift procedure and for several weeks thereafter. This will help protect the incisions as they heal and ensure the breasts stay in the proper recovery position. Once cleared by our surgeon, a soft support bra can be worn, but patients should avoid underwire bras for at least eight weeks. Once the breasts have fully healed, it is imperative to continue wearing a supportive bra on a regular basis. This helps to prolong the rejuvenated, lifted outcome and resist the gradual effects of the natural ageing process that will eventually continue in the breast area.

Contact Us
To schedule a consultation with Dr Craig Layt, or to learn more about breast lift surgery, contact our Gold Coast practice in Queensland today. We will be happy to answer any questions you have.